When looking at the contributing factors upon the health of US citizens, research quickly shows that medical care itself accounts only for 10-20%. The remaining 80-90% of contributors influencing health is attributed to one’s physical environment, socioeconomic factors, and health-related behavioral aspects – significant areas referred to as Social Determinants of Health (SDOH).1 For health plans, considering the 80% is a large piece of the picture when it comes to optimizing health outcomes.
The World Health Organization defines SDOH as the non-medical factors that influence health outcomes: “the conditions in which people are born, grow, work, live, and age, and the wider set of forces and systems shaping the conditions of daily life, including social, behavioral and environmental determinants of health.”2
Health plans now have the opportunity to support and fulfill Medicare social determinants of health with newfound, positive health outcomes for recipients and health care plans through the rising focus on social isolation and loneliness.
SDOH solutions – A 21st Century global topic
SDOH is a relatively young classification within public health and area of academic and political study. Starting in the early 2000s, the World Health Organization (WHO) facilitated the global discussion on the topic3 and developed the Commission on Social Determinants of Health. Their 2008 report provided a deep understanding of health equity and from a global perspective. Federal government agencies, health systems, educational institutions, and health advocates, among others, adopted the WHO social-determinants model and began using the language to discuss health and health outcomes.4
Since then, many organizations have adapted and expanded the WHO model of SDOH. Today, factors such as stress, discrimination, social integration, support systems, and community engagement are included, which is where social isolation fits as a contributing factor to the health of the individual. 4
Loneliness, social isolation, and health outcomes
Although both loneliness and social isolation have been a growing international concern as detrimental upon health, a deeper understanding of the negative effects of the loss of human connection has emerged from Covid-related lockdown restrictions and other outcomes.
Pre-Covid, the AARP reported in its 2019 article, “Is There a Medical Cure for Loneliness?”, “Certainly, physical and mental health issues can put you at risk for loneliness and isolation, but the evidence we have is independent of health status…Whether or not (a person is) healthy, those who are more socially connected live longer.”5
In the US, the topics have gained enough thrust that a bill to amend the Older Americans Act of 1965 to address social isolation and loneliness and for other purposes was introduced in the Senate in 2019.12

In a 2021 publication on the topics, the WHO states “Social isolation and loneliness are increasingly being recognized as a priority public health problem and policy issue for older people” and outlines the scale, impact, and harms of the conditions “which have been made more salient by the COVID-19 pandemic.”7
The WHO notes the conditions as “important, yet neglected, social determinants of the health of older people,” and states “A large body of research shows that social isolation and loneliness have a serious impact on older people’s physical and mental health, quality of life, and their longevity. The effect of social isolation and loneliness on mortality is comparable to that of other well-established risk factors such as smoking, obesity, and physical inactivity.” 7
The health care cost of loneliness and social isolation
Prior to Covid’s impact, in 2017 AARP published a landmark report which found the lack of social contact to be associated with an additional $6.7 billion in increased Medicare spending.10 In tandem with the AARP’s findings, a report by the National Academies of Sciences, Engineering, and Medicine identified social relationships as one of the five social risk factors to account for in Medicare payments.11
A 2019 report by Deloitte Insights, Addressing the social determinants of health for Medicare and Medicaid enrollees, stated Managed Care Organizations (MCOs) offering Medicare Medicaid services and Medicare Advantage plans (MA) play a critical role in addressing health-related social needs…and ensure that SDOH efforts remain patient-centered and integrated into patient care.13
According to the Coalition to End Social Isolation and Loneliness, social isolation and loneliness take a toll on physical and psycho-social health, leading to poorer health outcomes, higher rates of mortality, and higher health care costs.6 The National Academies of Sciences, Engineering, and Medicine 2020 publication Social Isolation and Loneliness in Older Adults summarizes the evidence base and explores how social isolation and loneliness affect health and quality of life in adults aged 50 and older, particularly among low income, underserved, and vulnerable populations.14
More recently, the CDC published a report in 2021 outlining recent study findings on the impact the conditions have on a number of health conditions.8 In the same year, a study published by Rise Health found SDOH linked to increase Medicare spending in multiple ways, commonly associated with chronic illnesses such as diabetes, heart conditions, and cancers.15
Help for Medicare with Z Codes – Coding for loneliness, social isolation, and SDOH
One tool available to health care professionals to capture data on the social needs of their patient population is the ICD-10-CM codes included in categories Z55-Z65, “Z codes,” which identify non-medical factors that may influence a patient’s health status used in medical billing.18
While available in 2016, Z codes adoption has been slow due to a lack of clarity on who could document a patient’s social needs, absence of operational processes for documenting and coding social needs, and unfamiliarity with the codes. Additional clarifications were made and approved in 2018 and 2019 defining “clinicians” as anyone deemed to meet the requirements, set by regulation or internal hospital policy, to document in the patient’s official medical record, in addition to documenting social (vs. medical) information.
Now, any clinician including, but not limited to, social workers, community health workers, case managers, nurses, or other providers, can document a patient’s social needs using Z Codes – including patient self-reported social needs.
Z Codes can enable more Medicare members who are experiencing the negative effects of loneliness and social isolation and its association with SDOH to gain access to care. Depending on the plan, Z codes can be used for either primary or secondary diagnoses which can help broaden access to and expedite delivery of care services for Medicare stakeholders and their broader communities.
In 2019, health care providers used Z codes for 1.6% of Medicare fee-for-service beneficiaries according to the Centers for Medicare & Medicaid Services.19
The 5 most utilized Z codes were:
- Z59.0 Homelessness
- Z63.4 Disappearance and death of family member
- Z60.2 Problems related to living alone
- Z59.3 Problems related to living in a residential institution
- Z63.0 Problems in relationship with spouse or partner
Z60.2 is a billable diagnosis code used to specify a medical diagnosis of problems related to living alone. It may be used to specify conditions or terms such as “lives alone; lives alone, help available; lives alone, needs housekeeper; lives alone, no help available; or no help available from lay caregiver.”
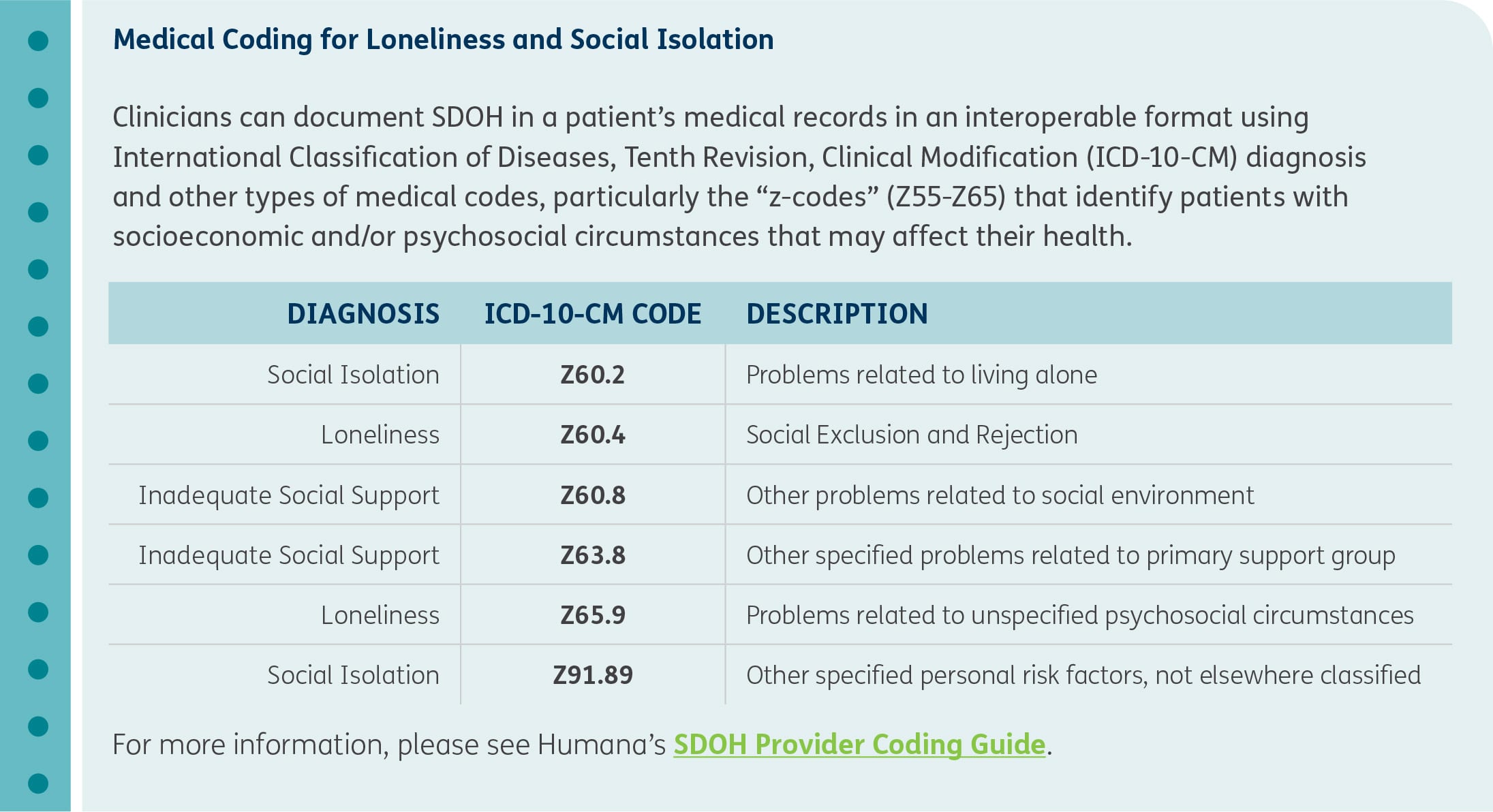
As a reference example below,21 in Humana’s 2021 coding publications, SDOH needs are listed as secondary diagnoses with guidance for clinicians to document Social Isolation using code Z60.2 (Problems related to living alone), and Loneliness under Z60.4 (Social Exclusion and Rejection – exclusion and rejection on the basis of personal characteristics, such as unusual appearance, illness, or behavior).20
Z code guidance chart
As Covid continues and the impacts of loneliness and social isolation become more well recognized as part of SDOH and predictors to health, Z codes can help broaden access to and expedite delivery of care and social services for traditional Medicare members, as well as Private health insurance stakeholders. Expanding provider awareness of Z codes can help support broader communities in dealing with disparities in health.
A simple innovation leads to closing gaps in care
For Pyx Health, addressing SDOH from a loneliness and social isolation perspective is a successful access point to bettering health outcomes for Medicare members plus increased engagement for health plans. Not only does their data show improved individual outcomes, independent research of their break-through solution has captured significant savings and return on investment (ROI) outcomes for health plans.
Through a novel, simple approach, Pyx Health blends direct human connection and a science-based mobile app experience. Their non-clinical, holistic care solution operates as a critical point of outreach to bridge Medicare members immediately with the resources that will help them most, at the most important time of need.
Pyx Health’s Compassionate Support Center staff, who are well-versed in mental health and SDOH training, onboard and engage vulnerable Medicare members. Most often during initial screenings through phone interviews or via the Pyx Health app, urgent SDOH or mental health needs are identified and addressed. Members receive direct access to the most appropriate and efficient forms of care through their community and health plans’ resources.
Pyx Health’s unique approach providing immediate, personal attention to Medicare members has created a ripple effect across other physical and high-cost healthcare utilization areas. 61% of Medicare members show a reduction in depression, and 60% of members show a reduced loneliness score, averaging a 36% drop in the acuity.16 As a free health plan benefit, evidence-based, in-app content increased member engagement with wellness activities 46%.16
Three independent studies of the program show positive outcomes including dramatically reduced high-cost emergency utilization and hospitalization 57%.16 By effectively solving members’ immediate needs, Pyx Health’s data shows positive outcomes for Medicare members so much so that it is now offered as a free benefit to Medicare members of four of the top five health care companies in the US.
As a successful, innovative model, Pyx Health can be looked to as a high-quality solution to the epidemic condition of loneliness and social isolation for those under Medicare coverage. Through simple, science-based technology and compassionate human connection, the program directly answers barriers outlined in AARP’s report of screening efficiencies and return on investment (ROI). The program also aligns with recommendations of a study conducted by the National Opinion Research Center (NORC) at the University of Chicago. Which calls for supporting “health plans in transforming the relationship between medical and social needs in health care delivery, potentially improving health outcomes and well-being for millions of Medicare beneficiaries.” 17
No age group is immune to becoming socially isolated and experiencing negative health impacts. But for Medicare recipients and insurance providers, the connection between loneliness, social isolation, and overall health is becoming more recognized as an important predictor of access to and engagement in health care, as well as factor in health outcomes. Loneliness and social isolation screenings are an innovative, successful means through which to address SDOH for Medicare recipients with positive, tangible health care outcomes.
References
1. Magnan, S. 2017. Social Determinants of Health 101 for Health Care: Five Plus Five. NAM Perspectives. Discussion Paper, National Academy of Medicine, Washington, DC. https://doi.org/10.31478/201710c https://nam.edu/social-determinants-of-health-101-for-health-care-five-plus-five/
2. Krohn, S. 2020. Addressing social determinants of health with data interoperability https://www.healthcareitnews.com/blog/addressing-social-determinants-health-data-interoperability
3. Wikipedia https://en.wikipedia.org/wiki/Social_determinants_of_health
4. Muttillo, E. 2020. Social isolation: A quiet social determinant of health; The Center for Community Solutions https://www.communitysolutions.com/social-isolation-quiet-social-determinant-health/
5. Daling, L. 2019. Is There a Medical Cure for Loneliness? AARP https://www.aarp.org/home-family/friends-family/info-2019/medical-cure-for-loneliness.html
6. 2021-2022 Policy Priorities; Coalition to End Social Isolation & Loneliness https://www.endsocialisolation.org/policy-priorities
7 Social Isolation and Loneliness; World Health Organization. ISBN: 978 92 4 003074 9 https://www.who.int/teams/social-determinants-of-health/demographic-change-and-healthy-ageing/social-isolation-and-loneliness
8 Loneliness and Social Isolation Linked to Serious Health Conditions; Centers for Disease Control and Prevention https://www.cdc.gov/aging/publications/features/lonely-older-adults.html
9 2021-2022 Policy Priorities; Coalition to End Social Isolation & Loneliness https://www.endsocialisolation.org/policy-priorities
10. Social Isolation: An Important Health and Public Health Issue and a Significant Cost to Medicare; Public Policy Institute. AARP. https://www.aarp.org/ppi/info-2018/social-isolation-event.html
11. Holt-Lunstad, J. 2020. Accounting for social risk factors in Medicare payment. Washington, DC: The National Academies Press. doi:
10.17226/23635. https://www.healthaffairs.org/do/10.1377/hpb20200622.253235/full/
12. S.2677 – Older Americans Social Isolation and Loneliness Prevention Act; 116th Congress (2019-2020) https://www.congress.gov/bill/116th-congress/senate-bill/2677/text?r=3&s=1
13. Josh Lee, J; Majerol, M; Burke, J. Addressing the social determinants of health for Medicare and Medicaid enrollees. Deloitte Insights https://www2.deloitte.com/us/en/insights/industry/health-care/applying-social-determinants-of-health-mcos.html
14 The Health and Medical Dimensions of Social Isolation and Loneliness in Older Adults. 2020. The National Academies of Sciences, Engineering, and Medicine. https://www.nationalacademies.org/our-work/the-health-and-medical-dimensions-of-social-isolation-and-loneliness-in-older-adults
15 Rosetti, T. 2021. SDoH linked to increased Medicare spending. RISE. https://www.risehealth.org/insights-articles/sdoh-linked-to-increased-medicare-spending/
16 Pyx Health data
17 Innovative Approaches to Addressing Social Determinants of Health for Medicare Advantage Beneficiaries; 2021. NORC, University of Chicago. https://bettermedicarealliance.org/wp-content/uploads/2021/08/Innovative-Approaches-to-Addressing-SDOH-for-MA-Beneficiaries-FINAL.pdf
18. Resource on ICD-10-CM Coding for Social Determinants of Health. American Hospital Association.https://www.aha.org/dataset/2018-04-10-resource-icd-10-cm-coding-social-determinants-health
19. Utilization of Z Codes for Social Determinants of Health among Medicare Fee-for-Service Beneficiaries, 2019. Data Highlight 2021. Centers for Medicare & Medicaid Services, Office of Minority Health https://www.cms.gov/files/document/z-codes-data-highlight.pdf
20. Social determinants of health Addressing patients’ social health needs ICD-10-CM SDOH codes included. Humana. https://populationhealth.humana.com/wp-content/uploads/2021/10/FINAL-LC14832ALL1021-A-SDOH-Coding-Flyer-Humana.pdf
21. Loneliness and Social Isolation Social Determinants of Health Issue Brief. 2021. PopulationHealth.Humana.com https://populationhealth.humana.com/wp-content/uploads/2021/10/SDOH-Issue-Brief_Loneliness_October2021-EXTERNAL.pdf